Driving Environmental Impact Through Daily EVS Operations
By integrating UV-C technology with manual cleaning, the team addressed potential gaps in disinfection, improved patient safety, and increased staff confidence. The increase in utilization, combined with strong ATP testing results and reduced HAI trends, demonstrates the value of UV-C as an essential infection-prevention strategy.

Best Practices for UV-C distribution
THE STRATEGY
Environmental Services (EVS) expanded UV-C light deployment beyond contact isolation rooms to include patient-ready rooms, ORs, L&D, Endoscopy, and targeted ED areas.
INTERVENTION
Process Change:
Scope Expansion:
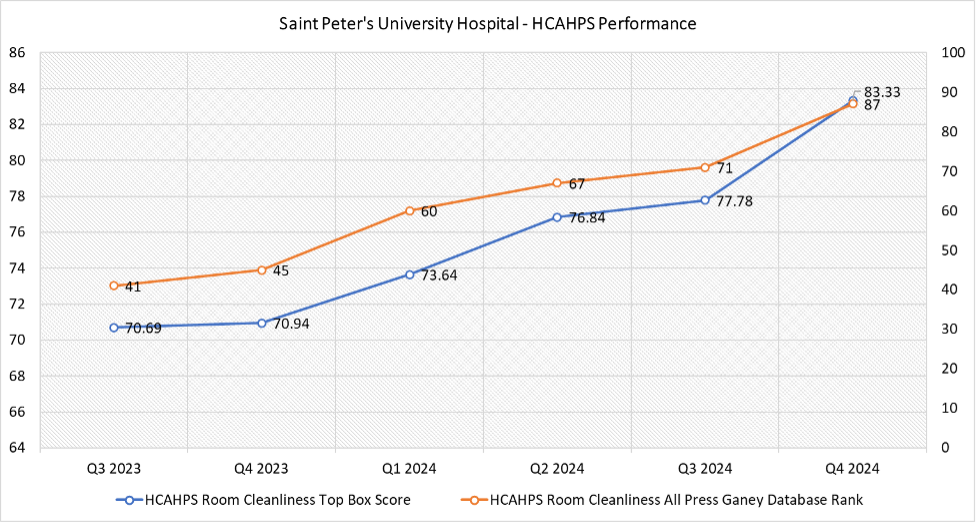
HCAHPS Outcomes